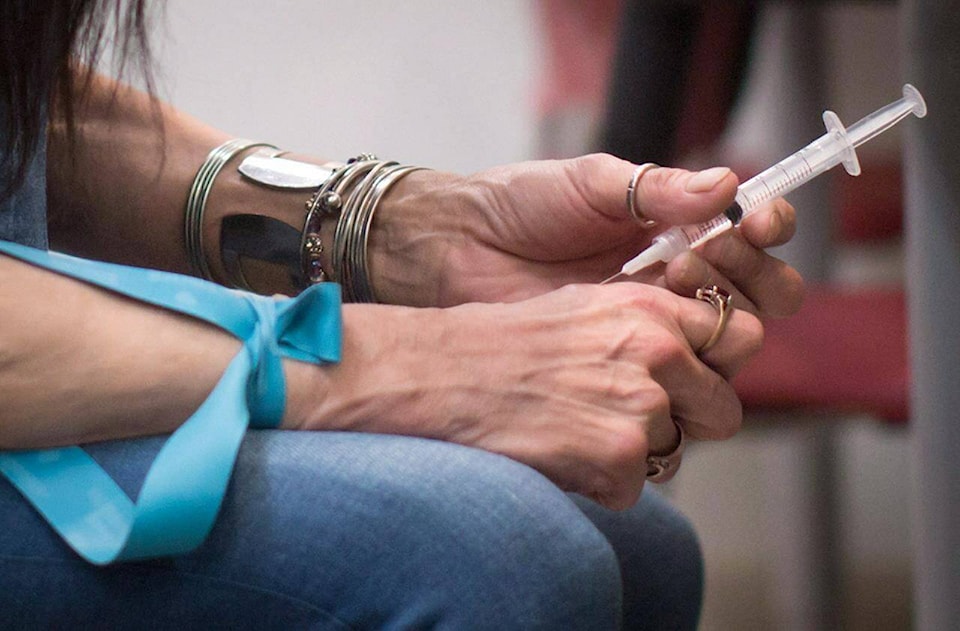
Peer-reviewed research is emerging about the possible impacts of British Columbia’s safer supply program, which provides prescription alternatives to toxic illicit drugs, with two studies in international medical journals casting the strategy in a different light.
One found the program was associated with a reduced risk of death from overdose and other causes among opioid-using participants, while the other concluded the strategy was associated with a significant increase in opioid overdose hospitalizations across the community.
The authors of the studies say the two sets of results aren’t contradictory; instead, they ask different questions about the policy introduced in 2020.
The safer supply policy has since become a lightning rod for critics, including federal Opposition leader Pierre Poilievre, who has pledged to shut it down if he becomes prime minister.
Shawn Bugden is an author of one of the studies, which found an almost 63 per cent “relative increase” in the opioid overdose hospitalization rate across B.C. after the introduction of safer supply. It was published in JAMA Internal Medicine in January.
He said in an interview there could be multiple explanations, including the diversion of safe-supply drugs onto the illicit market, which the study says could occur “for various reasons, including to purchase unregulated fentanyl.”
Increased toxicity of illicit drugs during the period of the study could also be to blame, but Bugden said there was no similar increase in Saskatchewan or Manitoba. Those provinces do not have safer supply and were chosen as controls for the study because they had comparable data to B.C.
The authors were not trying to imply “causality” between safer supply and the spike in overdose hospitalizations, said Bugden, dean of the school of pharmacy at Memorial University of Newfoundland.
“Is it possible that putting more opioids into the system is not necessarily the solution, even though a common-sense approach to suggest a safer supply of drugs would be helpful? I don’t think we really know those answers,” he said.
“But they’re not inconsistent with the fact that some individual people may benefit. I think we just need more in-depth follow up,” he added
He said “careful evaluation” was needed to make sure safer supply was working as intended.
“And on the other end of the spectrum, I think it would be absurd to indicate that our paper is definitive evidence that safer drug supply does not work.”
The study didn’t find a statistically significant change in deaths from apparent opioid poisoning.
Dr. Paxton Bach is one of the authors of the other study, published in the British Medical Journal in January. It concluded that one day or more of prescription opioid dispensation was associated with “significantly reduced all-cause mortality” as well as overdose deaths over the next week.
He said mortality reduction within a one-week timeframe may not seem significant, but the benefits add up.
“If somebody stays on this program for six weeks, or 12 weeks or 24 weeks or a year, then that risk (reduction) really starts to accumulate,” he said.
“The total reduction really depends on how long you’re participating.”
Bach said the JAMA studydemonstrated the possibility of an increase in opioid-related hospitalizations in B.C. compared with other provinces.
“But I think it’s very difficult to convincingly link that to the prescribed safer-supply policy,” said Bach,an addiction medicine physician at St. Paul’s Hospital in Vancouver and co-medical director of the B.C. Centre on Substance Use.
He said the other researchers were clear about their use of an approach that he said assumed everything would have stayed the same in the absence of safer supply. “I think that is, in these times, a very tenuous assumption,” Bach said.
“There are many things changing these days in our health-care system that are not necessarily similar between provinces, and in particular, as far as the toxic drug crisis goes, we are all experiencing rapidly evolving versions of the crisis.”
Bugden said of the BMJ study that it was “puzzling” that the research didn’t register benefits for acute care visits, and one week was a “narrow window” to examine.
“We really want to see whether, in the long term, this is resulting in (fewer) deaths at the individual level. And if that works well enough, then we should see it at the population level, eventually, as well,” he said.
Bach said it was “unreasonable” to expect the data to register changes at the population level when fewer than five per cent of people at the highest risk of overdose in B.C. were accessing safer supply.
About 70,000 people had signals of opioid use disorder and 5,356 of them received opioid dispensations during the BMJ study’s period.Among nearly 42,000 people with stimulant-use disorder, 1,061 received safer-supply stimulants, the study says.
B.C. declared the opioid crisis a public health emergency in April 2016 and since then, more than 14,000 people have died, most of them from highly potent fentanyl.
A statement from the Ministry of Mental Health and Addictions said the BMJ study showed safer supply was preventing deaths and helping people stabilize their lives.
Asked about the JAMA study, the ministry said it “overlooks other factors that influence hospitalizations,” such as the toxicity of the illicit drug supply, as well as admitting practices and the availability of health-care services.
The issue of potential drug diversion from the safer supply system has been in the national spotlight since police in Prince George, B.C., issued a news release last month saying trafficking investigations were finding increasing amounts of medications used in the program.
The statement triggered criticism of B.C.’s policy from Poilievre and from Alberta Premier Danielle Smith, who worried the drugs would end up in her province.
At the time, B.C. Solicitor General Mike Farnworth said Mounties had told him there was no evidence of widespread diversion of safer-supply medications.
On Monday, RCMP in Prince George announced two people had been arrested over allegations they were trafficking in safer-supply drugs. The Mounties said the suspects were allegedly seen “exchanging illicit drugs for safer supply drugs.”
READ ALSO: B.C. safe supply advocates rally to mark 7 years of toxic drug crisis
READ ALSO: Widespread safe supply drug diversion in B.C. ‘simply not true’: Farnworth